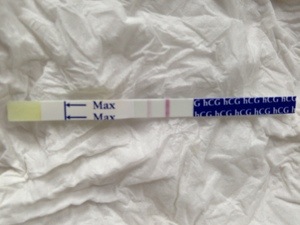
Please think twice before you say things like this.
We’ve all had to deal with numerous hurtful comments from friends or family or medical professionals. Here’s a list of comments that have been said to me personally that I have found hurtful and destructive, even though they might have been well-intentioned. I have added the responses I wished I had been able to come up with at the time but in the shock of the moment these words sadly went unsaid.
Pretend the babies weren’t real. Try to forget as though they never happened
Errr, no can do I’m afraid. At the sight of a positive test every mother has already named that child, watched them take their first step, taken them to their first day of school, helped her pick out her wedding dress. It is real. A tiny heart beat in an ultrasound is very real. You can’t just switch off your desire to be a parent like that.
Well at least you got a little further this time around
This is not a consolation prize. A loss is significant at any point, at any age
Go on holiday, that’s how my friend got pregnant
Yes everyone has that friend who went away for a few weeks only to return to a blissful and straight-forward pregnancy. Trust me, if a couple of weeks on the beach was medically proven to allow me to carry my baby to term without complication, I would be the first in line.
Do you want to spend time with my baby instead to make you feel better?
No I do not. While I am thrilled that you and your baby and happy and healthy, this does not mean that your baby will take my pain away.
Maybe you should gain some weight
OK, sure there is an ideal BMI for conception and maintaining a pregnancy but come on, have you seen how I micro analyse every gram of protein to make sure I am getting the magic 75g daily? Or watched me count up the exact quantity of my “5 a day” veggies? Or heard me tell you that I cannot eat fruit or cold food because my doctor of traditional Chinese medicine tells me it will sabotage my kidney function? Trust me, I am already doing everything I can.
I’m sorry you are jealous of my pregnancy / new baby
Let’s get one thing straight. This isn’t about you. Don’t insult either of us by suggesting that that your happiness is causing my sadness. Because you know as your friend I am thrilled for you. But that doesn’t make my situation any less painful or traumatic. I deserve to have a child just as much as you do.
You just need to relax
Seriously, lack of relaxation time is not the reason why my body is spitting out my babies one after another. Don’t insult me.
Pretend like it’s just a dream and that everything will be fine when you wake up
Yes it is like a dream. Imagine the most horrific nightmare that you can’t wake up from, that gets scarier and more exhausting and more traumatising as time goes by. Please do not belittle what I going through by comparing it to an experience that isn’t real.
Everything happens for a reason
Even if you do believe this, it does not help. What reason would this be? Why am I being punished? Because I don’t deserve to be a mother? Because I delayed trying to start a family? What master plan is this a part of? Please don’t suggest that fate has had anything to do with this.
What’s wrong with you?
Look I know there is probably a lot wrong with me but your comment implies I want to talk about all the details. Please appreciate that I confided in you about my unfortunate situation but respect my privacy and trust that if I wanted to share it with you I already would have.
Oh she wants to have a baby or something and is jealous about us being pregnant so now she doesn’t want to hang out anymore
If I’ve confided in you that I’m going to have to take a few steps back from our relationship while I come to terms with my grief of having yet another pregnancy loss please don’t go relaying that information to everyone you (and I) know. If you don’t understand why I’ve needed to distance myself from your growing belly then it’s just as likely everyone else you tell that way won’t either. Please respect my privacy. Allow me to tell people when and the way I want to tell them. Understand that it might take me some time to adjust to the concept that you are getting what you want and I am continually denied it. I don’t want to feel this way but right now avoiding you is the only thing I can do to maintain some level of self preservation.
Cheer up
Sure thing, no problem. What’s the bright side? Look we can’t just snap our fingers and make all this hurt and anguish go away. I might not smile for a long time. As a friend you should respect my need to grieve and give me the space and the forum to do that.
I don’t understand why you won’t just have a few drinks, you will feel better
After years of trying to cleanse my body in order to make it more a more pleasant and habitable home for my future child, going out and getting smashed isn’t going to improve my situation. As a friend I would hope that you trust me to make the right decisions for my body.
I told you to follow my advice
I had to throw one in here from the medical community. Pregnancy loss is one of the most stressful experiences for any woman. She does not need to have her hand slapped by you for not following every single ounce of your protocol. Losses occur for many reasons but any woman who desires a child of her own would never willingly cause the death of her baby. She does not deserve to be blamed for losing her child. She is human and can only do as much as she can do.
At least you CAN get pregnant
How many times have I heard this one. Yes, medically speaking this may be a positive sign. However, emotionally there is no comparison to the highs and lows that accompany recurrent pregnancy loss. When there is no reason to explain your losses occuring over and over again. When you nearly retch with joy and fear at the sign of another positive pregnancy test. Will this one be lost as well? How long will this one last? Will I ever get to meet this child?
You are so lucky you don’t have kids
Really? And would you give it all up? I already know that babies can be hard work, that my life will change forever, but shouldn’t the fact that I am trying to achieve this relentlessly over and over again tell you that yes I sign up to all that? You know you are incredibly fortunate, so don’t pretend any different when I’m around. This is not the right thing to say to someone who is unable to have a child.
There’s always IVF
Yes there is and IVF works wonders for a lot of people. But it is not a band-aid solution for everyone. Conception is not the problem in recurrent pregnancy loss. It’s maintaining a pregnancy. Yes, I know the difference.
Well you have a sister
A response when I was told that I should consider egg donation. Egg donation is a wonderful option that helps many people achieve their dreams of having a child. But right now I need you to understand that I want to exhaust my options of having my own child first.
What about adoption?
Adoption is a great solution for many people struggling with infertility and recurrent loss to allow them to have the family they have always dreamed of. And it very well may be an option I consider at some point down the road but right now I need a friend who understands my need for my own biological child, that I’m not ready to give up that hope, and that I want to interrogate the medical system to finding a solution for me to achieve this. Don’t give up on me, I need your support.
Maybe you should have started sooner
Yes maybe we should have. Trust me, I regret delaying trying for a child everyday but you can’t say for sure that 5 or 10 years ago we wouldn’t had to endure the same struggles we are going through now. I don’t need to be made to feel like I am to blame for our heartache.
You have plenty of time left
I wish that were true. We all know it gets more difficult with age. We know there is an increased risk of ovarian failure, of chromosomal abnormalities, of pregnancy loss. Please don’t sugar coat the future.
It will happen next time. Don’t give up. Stay positive
Will it? Should I? Promise? This may sound reassuring when it comes out of your mouth but you probably realise that it might not ever happen. When there is no medical reason for multiple losses it does start to feel like it will never happen, and that is a normal response from someone going through this kind of scenario. We don’t want our feelings to be dismissed, we need you to listen to our fears and our concerns. And if it does all become too much and in the end we decide to give up the fight, we don’t want to be punished for not trying that one last time.
Get on with your life. Don’t dwell on the bad things.
I wish it was that simple. I am not likely to get over this. This pit of emptiness and self-loathing will likely remain with me for the rest of my life, regardless of whether I ever get the opportunity to have a family of my own. Believe me, I see the destruction this hardship has caused to my emotional wellbeing, to my relationships, to my daily motivation, and wish nothing more than to reverse it. But I am a different person now and the loss of my five babies will stay with me for the rest of my life.
<